In case we need more reasons to take our sleep health seriously, reduced or poor-quality sleep even has negative effects on your oral health.
Many of those who experience chronic poor sleep are suffering from either insomnia or sleep apnea. These conditions negatively impact your daytime function, reduce your quality of life, and can result in numerous long-term health conditions.
Insomnia
Insomnia affects anywhere from 10-30% of the population. Chronic sleep loss is linked to an increase in the incidence of periodontitis— a huge 36% increase. Reduced sleep duration means that there is less saliva production, which is essential to healthy teeth and gums. Many people also get out of bed and get a snack when they have trouble falling and staying asleep. Night Eating Syndrome, or NES, not only contributes to depression and weight gain, but can also lead to the breakdown of tooth enamel, since most insomniacs do not take the time for teeth-brushing after their midnight snack.
Sleep apnea
Another common sleep disorder is sleep apnea. Obstructive sleep apnea, or OSA, occurs when your airway either partially or fully closes while you are asleep. Each time this happens, your oxygen levels drop, you wake up without remembering it, or both in many cases. This can also lead to an array of poor health outcomes, many strongly linked to oral health.
Many people with obstructive sleep apnea tend to breathe through their mouths, since this is the path of least resistance for airflow. Chronic mouth-breathing is linked to everything from bad breath to changes in facial structure. There is also a 50% chance that someone with bruxism (teeth-grinding) has OSA—in fact, it’s been shown that those with mild or moderate OSA have more severe bruxism than those with severe OSA.
Symptoms of sleep apnoea:
- Snoring
- Episodes of not breathing during sleep- this can be reported by others
- Gasping for air during sleep
- Waking up with dry mouth
- A headache in the morning
- Difficulty staying asleep
- Excessive daytime sleepiness
- Difficulty paying attention while awake
- Irritability
We recommend that you speak to your dentist if you suspect that you have sleep apnea. If diagnosed, you can be treated with either an oral appliance therapy or CPAP.
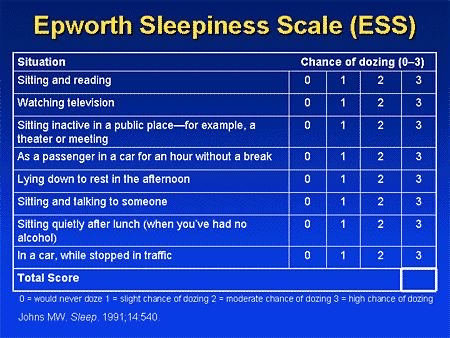
The treatment is planned according to the severity of symptoms and grade of obstructive sleep apnoea which is calculated according to the Epworth Sleepiness Scale (ESS) and other factors.
Non-Surgical Treatment:
Conservative treatment is best for people with mild sleep apnea.
- Weight loss
- Avoid alcohol or sleeping pills etc
- Sleep in position with least snoring with help of pillows or support – side sleeping is generally better than on your back.
- Use nasal sprays or decongestants if you have nose or sinus issues.
- Yoga can increase your respiratory strength and help the flow the oxygen.
- Use a humidifier to open the airways and reduce congestion, promoting clearer breathing. Consider adding lavender, mint or eucalyptus.
- Singing exercises.
- 10 exercises for tongue, jaw and throat. Click here to view these:
https://sleep-land.com/10-sleep-apnea-exercises/
Mechanical aids:
- C-PAP (Continuous Positive Airway Pressure)
When the muscles of your throat relax and the muscles collapse the airway causing difficulty in breathing in such conditions the machine pushes positive air through a mask causing relief from the sleep apnea and even reducing or resolving snoring completely.
- Oral devices such as a mandibular advancement and tongue stabilisation device
These work by repositioning your lower jaw or tongue forward to keep your airways open while you sleep.

- The last treatment option is surgery.
This includes septoplasty or functional endoscopic sinus surgery (FESS), UvuloPalatoPharyngoPlasty (UPPP) and tonsillectomy.
Sleep is the basic necessity for every human being – talk to your dentist if this is something you suffer from.






